For decades, Polycystic Ovary Syndrome (PCOS) has been a leading cause of infertility and hormonal imbalance worldwide. However, a major shift is underway in the medical community to rename the condition Polycystic Metabolic Ovarian Syndrome (PMOS).
This name change isn’t just about semantics; it is a critical effort to improve diagnosis, treatment, and patient understanding of a condition that affects far more than just the ovaries.
Why the Change to PMOS?
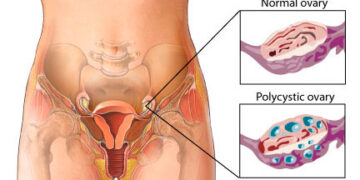
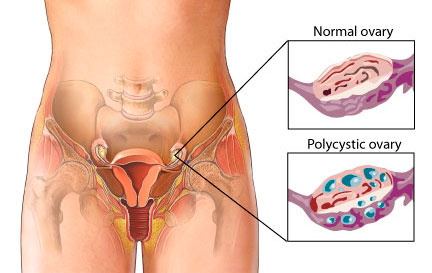
The term “PCOS” has long been criticised by patient advocates and endocrinologists for being misleading. The original name suggests that the presence of ovarian cysts is the primary symptom. In reality, many women with the condition do not have cysts, while many with cysts do not have the syndrome.
By adding “Metabolic” to the name, medical professionals are highlighting the root causes and risks associated with the disorder, including:
-
Insulin Resistance: A core component where the body struggles to process blood sugar.
-
Metabolic Syndrome: Increased risk of type 2 diabetes and cardiovascular disease.
-
Hormonal Imbalance: Excess androgen (male hormone) levels that lead to acne and hair growth.
The Impact on Women’s Wellness
The transition to PMOS is expected to change the “wellness” conversation around the disorder. For years, patients felt dismissed when their concerns focused on weight gain, fatigue, or mental health rather than pregnancy.
1. Better Diagnostic Criteria
The name change encourages doctors to look at the “whole person.” Instead of focusing solely on an ultrasound of the ovaries, providers are now more likely to screen for metabolic markers like fasting glucose and cholesterol levels early on.
2. Tailored Treatment Plans
Treatment is shifting from a “one-size-fits-all” approach (often just prescribing birth control) to comprehensive metabolic management. This includes:
-
Lifestyle Interventions: Diet and exercise tailored to insulin sensitivity.
-
Medication: Use of insulin-sensitising drugs like Metformin.
-
Mental Health Support: Addressing the link between metabolic health and anxiety/depression.
What This Means for Patients
If you have been diagnosed with PCOS, this shift to PMOS is good news. It validates the systemic symptoms you may have been experiencing, such as stubborn weight gain or extreme fatigue, as clinical components of the syndrome rather than personal failures.
As the medical community adopts this new terminology, patients can expect more comprehensive care that prioritises long-term health and prevents metabolic complications later in life.